- Home
- Severe Burns
Severe Burns
Severe burns are those 2nd or 3rd degree burns of 20% or more of the body's surface. These patients will require intensive care.
Only certain hospitals have a Burn Intensive Care Unit.
By the time you read this, your loved one should already be in such a place or being transferred to one.
Severe Burn Causes

House fires, car or truck accidents, smoking in bed, especially with oxygen, all lead to the burn unit.
Escaping a house fire; but returning for a person, pet or object often leads to severe burns.
Electrocution is a type of burn. Industrial explosions cause very serious burns. Large bonfires, involving alcohol, will send victims to the Burn ICU.

ICU Treatment of Severe Burns
Severe burns cause the body to immediately lose large amounts of fluid. Intravenous fluids are started at a rapid rate to catch up and stay with the fluid loses.
This means in the first 24-48 hours major swelling develops. The larger the burn, the greater the swelling. Sometimes you may not recognize your loved one.
This swelling is common and the doctors and nurses know how to deal with it.
While the fluids are going in, the nurses will be cleaning the burn wounds and applying various dressings. They will be changed 2-3 times a day.
Burns and burn wound dressing changes are painful. so the third thing immediately being done is pain medication.
These wounds are painful enough to require narcotics either from time to time or continuously.
As soon as possible Physical Therapists will work with your loved to prevent joints from freezing up.
Standing and walking will be started to minimize deconditioning due to the bed rest.
Nutrition is a very important part of burn recovery. Most severely burned patients cannot get in the necessary amount of calories on their own.
If unable or on a ventilator, a small tube will be threaded through the nose into the intestinal track. The nutrition can then be continuously given.
Burn Surgery
The first surgery will usually be done in the first 48-72 hours. The plan is to remove the burned area and if possible cover it with a skin graft from the burned patient.
Larger burns will probably require multiple operations to get all the burns removed and covered.
Large burns may not leave enough good skin to apply a skin graft. Some form of artificial skin or from a donor will be used. Pigskin is also commonly used for this.
The artificial skin, pigskin, or donor skin are all temporary. Over time, they will be replaced, hopefully with your loved one's own skin.
All of this will require multiple surgeries and over a long period of time.
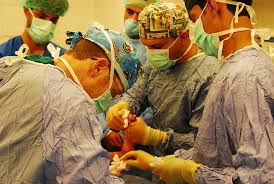
Burn Complications
Severe burns almost always lead to complications during the ICU stay.
Burning materials, particularly in a house fire, can produce carbon monoxide.The burn victim can develop carbon monoxide poisoning.
The carbon monoxide can cause loss of consciousness. If so, a ventilator will be needed.
Large, severe burns can lead to cardiac arrest at the scene, CPR will be necessary.
Closed space fires, such as a house, can cause smoke inhalation.
These patients need the ventilator and are sicker than someone else with the same size burn; but no smoke inhalation.
Smoke inhalation means pneumonia is more likely as well longer times on the ventilator.
Medications are directly placed down the breathing tube to prevent secretions from blocking the air passages.
Burn wounds can develop infection.This often causes the skin graft to fail and be removed. Antibiotics and aggressive wound care are necessary.
The skin is actually the body's largest organ. When severely burned, it can easily cause failure or poor function any of the other organs.
The kidneys are at risk, especially if there was any underlying kidney issues. Dialysis(artificial kidney) may be needed for several days or weeks.
In some cases the skin grafts do not take. They require removal and replacement when it looks as though the burn site can accept a new graft.
Pain control and sedation can become difficult . Several different medications may be necessary to get the right level of sedation.
Age can play a role in complications. Most elderly patients over 70 years have some issues. Even a small burn can cause major organ failure.
Even though the burns are small in size, this type of patient may need Burn ICU care.
Longer Term Complications
Long stays in the Burn ICU with continued need for narcotics can cause problems after discharge from the ICU.
Narcotic withdrawal may take several months and may not always be complete.
The nurses and doctors are well aware of this and try very hard to minimize and discontinue those medications as soon as possible.
If the ventilator is required for more than 7-10 days a tracheostomy is usually done.
Removal may not occur even when off the ventilator until your loved one can cough up their own secretions and no longer require suctioning.
While not directly part of ICU care, burn scarring is a major concern. After ICU discharge many operations may still be necessary to deal with this.
Burn Survival
Most Burn ICUs use a scoring system to predict outcome. It is based on the burn size, patient age and whether an inhalation injury is present.
It takes into account the likelihood of complications happening during the course of treatment.
The score cannot predict the length of ICU stay. In general, the larger the burn and the more complications, the longer the stay.
Unfortunately some patients arrive with very large burns which clearly are not survivable.
Once that is clear to all family members, comfort measures with adequate sedation and pain control are the primary care modes. The Palliative Care Team can be called in.
Questions to Ask
- What is the burn size?
- Is there an inhalation injury?
- What does the scoring system say about survival?
- If your loved one is not awake, ask about the possibility of carbon monoxide poisoning.
- When do you plan to operate?
- Will artificial skin coverage be necessary?
- If all goes well, how many surgical procedures do you think will be needed?
- What type of scarring do you expect?
- When do you think narcotics can be stopped?
- How likely do you think kidney failure or pneumonia will develop?
- Will rehab be necessary?
- If our loved one cannot survive, what should we be doing and what will you do?