- Home
- ICU Nurses and Others
ICU Nurses and Others
Your first encounter will be an ICU nurse. At first, the ICU nurses and others can be intimidating. Who are all these people? What do they do?
It may look confusing; but soon you will see each person is part of a team with a specific job.
All are devoted to providing your family member with the best care and chance for recovery.
ICU Physician Assistants & Nurse Practitioners
Both these groups have had several years training in caring for critically ill patients. They act as an extension of the ICU doctors and are directly under their supervision.
They are often called a PA or NP or Extender. Several times a day they will round on your loved one. This includes a physical examination and and receiving an update from the bedside ICU nurse.
Lab results, cultures, scans and x rays are reviewed. These will be discussed on rounds and at other times with the ICU doctor. A specific treatment plan will be made.
The PA's & NP's ensure the care plans are followed. They will keep the ICU doctor informed and up to date, even if he or she is not currently in the unit.
The PA and NP are trained to do most of the usual ICU procedures; such as placing tubes or intravenous lines. They can also order all lab studies, x rays and scans.
Except in an emergency, the ICU doctor may help and be present.
These extenders will almost always be happy to answer your questions and help keep you informed. They may go over with you any procedure consents which may need to be signed.
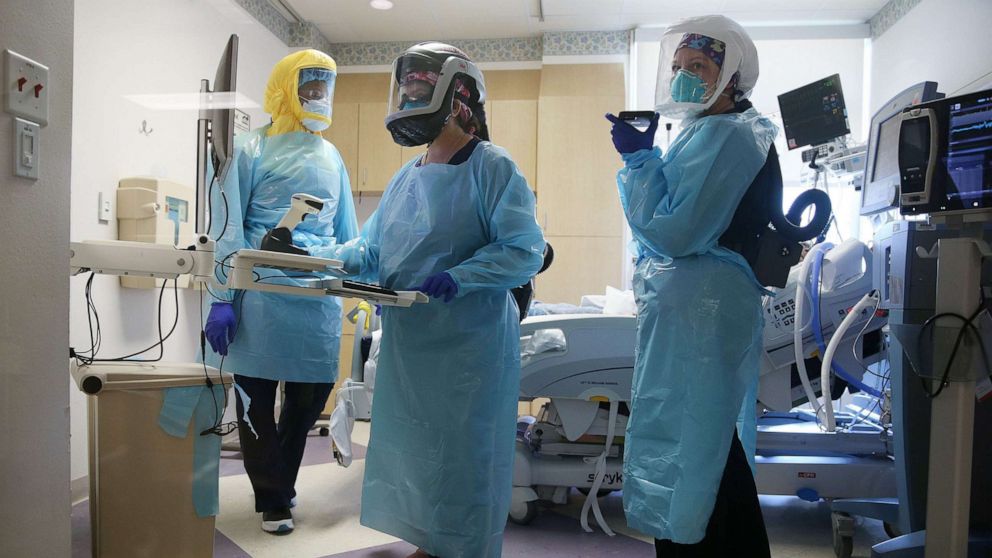
Below are Physician Assistants busy in the ICU
The ICU Nurse
All of your loved one's care in the ICU revolves around the bedside nurse. In most ICU's this nurse cares for one or at most two patients.
Very sick or newly arrived patients may have more than two nurses at the bedside until things stabilize.
This nurse will be constantly with your loved one throughout the shift. He or she can and will update you on what has previously happened and what is planned.
The nurse monitors and collects all vital signs and other measurements. He or she will inform the ICU doctor or extenders about any significant changes in the patient's condition.
This person is responsible for keeping your family member cleaned up and bathed. The nurse follows the doctor's orders, delivers and adjusts all medications.
This is particularly important when it comes to sedation and pain control.
The ICU nurses will keep your family member properly positioned in bed and when indicated will help get him or her to a chair or aid with limited ambulation.
Some hospitals have a Lift Team to help with these moves and save the nurse's back.
The ICU nurse will usually be the go-to person for any issues you might have.
The nurse will usually accompany your loved one any time they need to leave the ICU unit for a test or procedure.
Respiratory Therapist
Most ICU patients will require a ventilator for at least part of their ICU stay.
This is the role of the Respiratory Therapists. They are specially trained and certified to operate, adjust and trouble shoot the ventilator.
In most ICU's the therapist will be responsible for eight to twelve patients.
The ventilator adjustments are made based on orders by the ICU doctor, PA or NP. Some changes may be made based on previously developed protocols.
An unstable patient may require many changes in a short period of time. A more stable one may not require any new changes over a 24 hour period.
The therapist will be by to check the ventilator at least every two hours. He or she can and will suction secretions out your loved one's breathing tube.
The therapist will always accompany your loved one on any transports to other places in the hospital.
Respiratory Therapists have an important role in weaning the patient off the ventilator. The longer the time on the machine, the slower and more difficult the process.
In smaller ICU's, in an emergency, the therapist may be responsible for placing the breathing tube.
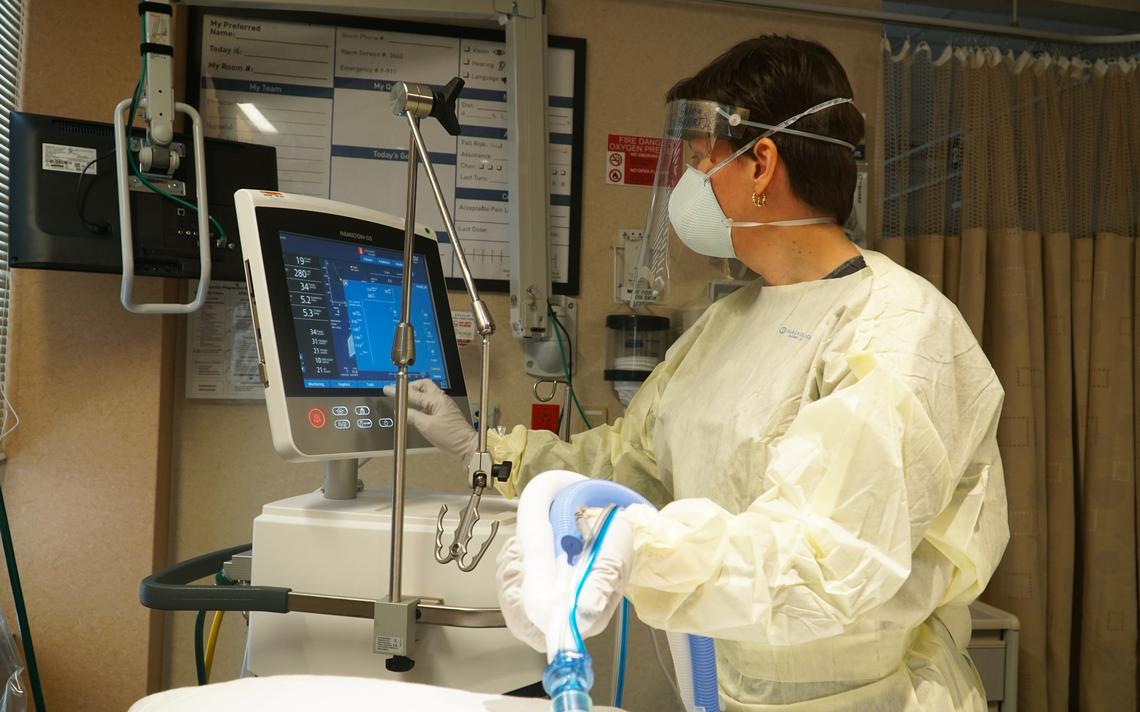
Below, a Respiratory Therapist adjusts a ventilator
Social Worker
If your loved one spends more than 24 hours in the ICU, you will no doubt come into contact with the Social Worker.
This person will be an invaluable and ongoing resource. He or she will walk you through the insurance, Medicare or Medicaid funding processes.
The Social Worker can help you to find a place to stay or aid with transportation for you to and from the hospital.
Very often the Social Worker will arrange a conferences for you and your family members with the ICU doctor.
This person can also help arrange transportation home for any family members in the military. He or she can alert an employer of your family member's unexpected illness and probable time away from work.
The Social Worker can help with any religious support. He or she will know the representatives of the various faiths and which ones come to the hospital.
When times are tense between your family and some staff members or doctors, the Social Worker is a very good person to help settle things down. This even applies to disputes between family members.
The Social Workers can be a real resource when dealing with death or a decision to stop care. They can arrange Hospice and/or palliative care either in the ICU or at a specialized facility.
The Social Worker are there for you. Take advantage of all their expertise and experience.
Sometimes emergency patients come to the ICU, and are unidentified. This social worker will use detective skills to identify the patient and notify the family.
Physical Therapists
If a critically ill patient does not have some daily physical activity, their joints can freeze and not move. This happens due to calcium collecting in the joint spaces.
ICU patients cannot do a lot of physical activity. Often they are on a ventilator or sedated.
At the vey least, Physical Therapists, who are also specially trained and certified, will perform passive motion on all the major joints; elbows, shoulders, knees, and hips.
This prevents the joints from becoming stiff and unusable.
For less sick patients, the therapist will work on standing and walking. Walkers or other devices help with this. The main goal is to keep the patient moving.
The physical therapist may ask some family members to become involved. The family can usually be taught to do some of the simple things such as passive motion.
Doing these several times a day, when the therapist cannot be there, will help the joints remain nice and loose.
A Physical Therapist helping an ICU patient maintain arm tone & strength
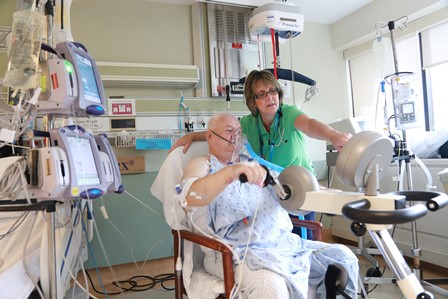
Occupational Therapists
These are the people who help with some of the motor skills, especially the hands. Sometimes after injuries or burns a particular arm or leg may need work.
This might include specific exercises, splints or special dressings.
Occupational Therapists can also help with communication when patients have a breathing tube or tracheostomy in place.
After a stroke, occupational therapists will help patients re-learn daily activities such as eating, bathing, writing and even using the phone or TV.
They can help to ensure patients have the kinds of music or TV shows they like. Some patients may be able to enjoy audio books or pictures of family members.
Dieticians
Most critically ill patients cannot eat normally as they do at home. To heal after a major illness, surgery or trauma, the diet needs to be very specific.
Protein is necessary to heal and improve the immune system. Also, patients require protein to heal wounds and to prevent muscle breakdown.
Unlike the typical starvation diet where the body uses fat as the major source of energy, critically ill patients obtain their energy requirements from protein.
The Dietician's role involves designing a specific diet to meet each patient's energy needs. These change with the specific illness, age, body size, sex and other factors such as sepsis surgery or pneumonia.
Most times, the nutritional needs for your loved one will be in a liquid form. It's continually given through a small feeding tube inserted through the nose and ideally into the small intestine.
Long term patients may have the tube directly inserted through the abdominal wall into the small intestine.
The Dietician will come by early in your loved one's admission and assess his or her needs. Feel free to ask questions.
Various lab tests determine how well the nutritional needs are being met. Adjustments are done when indicated by the lab results.
These are the times when you are likely to again see the dietician,
Pharmacists
You may not be aware of the ICU pharmacists. They often are on rounds with the doctors. They ensure that all the medications will not harm your loved one.
The Pharmacist helps choose the appropriate medications and ensure the correct dosage is given and on schedule.
Speech Therapists
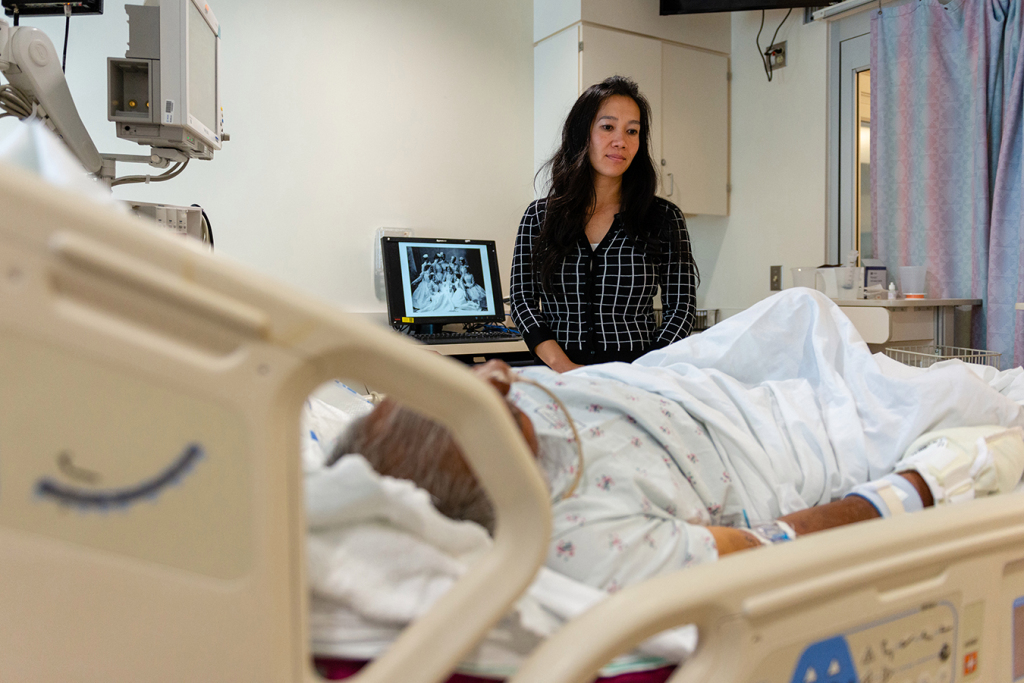
The Speech Therapist has two major responsibilities in the ICU. Patients on ventilators cannot talk; but need to communicate. The Speech Therapist uses bedside computers and other devices to help with this issue.
Another role for the Speech Therapist is to evaluate your loved one's ability to swallow. If unable, food can go directly into the lungs and cause pneumonia.
This is a situation for the previously mentioned feeding tube. Various tests including fluoroscopy help evaluate the swallowing mechanism.
As improvement occurs, the same tests can indicate when the feeding tube can be safely removed and a normal eating can be restarted.
Housekeeping
These are the unsung heroes; often not noted nor appreciated. However if they fail to come to work, it won't be very long before the rest of the staff notices their absence.
Without them, rooms cannot be thoroughly and rapidly cleaned to prepare for the next admission, which could be at any time.
A room with full trash cans, a dirty floor following a procedure, or other messes does little to improve your or your family member's mental health or confidence.
The housekeepers may not say much; but experienced ones know how each patient is doing. And they care.
They are definitely an important part of your loved one's team.
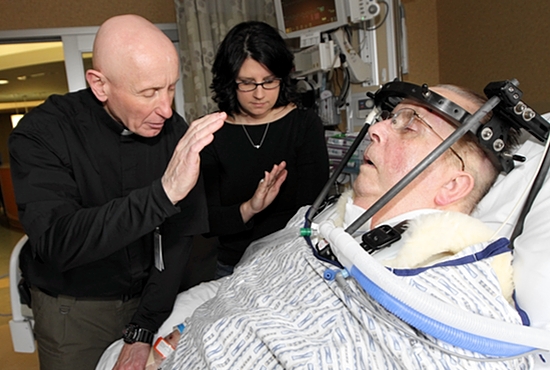
Spiritual Care
Patients in the ICU come from many many different Faith backgrounds. Most ICU's have a list of representatives from a large number of these diverse religions.
Some families may wish to bring their own spiritual advisor. Others are comfortable with the ICU recommendations.
The Social Worker will often be the one to arrange these visits. They can also fill a role when no spiritual advisor is requested.
In an emergency the spiritual advisors are welcome at any time. They can help the family, patient and ICU staff deal with a very emotional and difficult situation.
Gathering around the bedside for prayer can be very comforting for the patient and family members.
A hospital chaplain at the bedside of an ICU patient.